

Breast Reconstruction in Albania
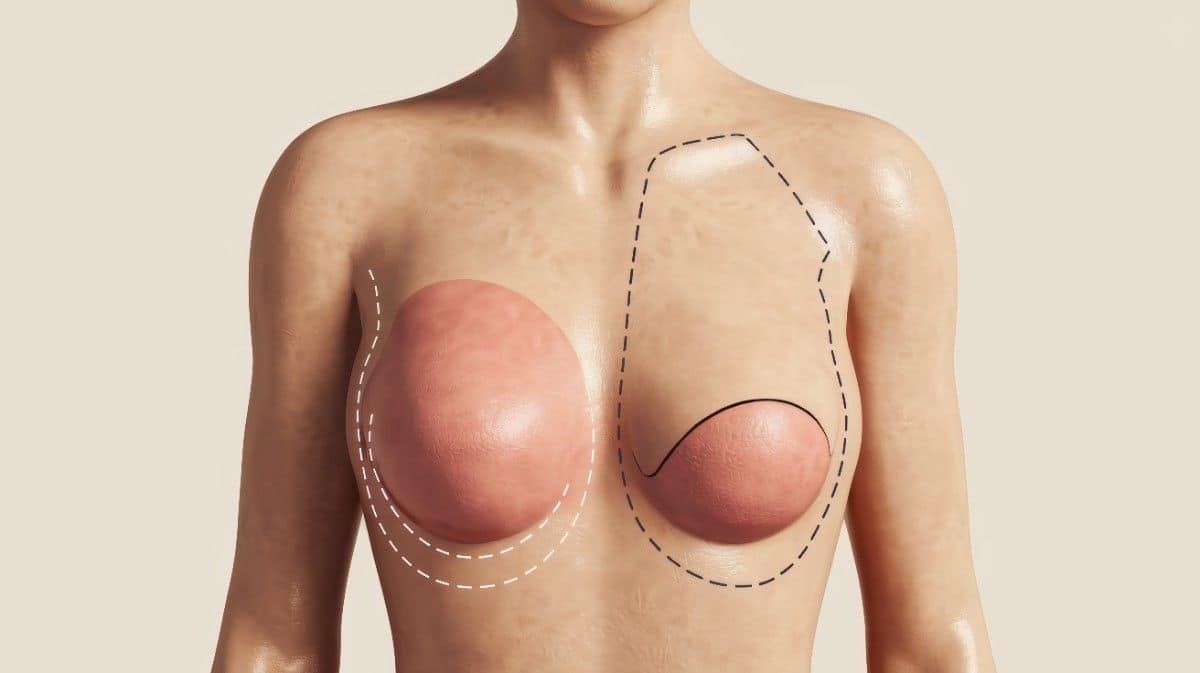
Breast Reconstruction at Hygeia Plastic Surgery in Tirana
Mastectomy is often necessary to treat breast cancer, but the loss of a breast can have a lasting impact on body image and emotional wellbeing. Breast reconstruction restores breast shape and symmetry and helps many patients feel whole again after treatment.
At Hygeia Plastic Surgery in Tirana, Albania, we perform breast reconstruction using implant-based techniques or the patient’s own tissue. Each case is planned individually, taking into account cancer treatment, anatomy, tissue quality, and long-term outcomes. Reconstruction is not medically required, but for many patients it plays a critical role in recovery.
Reconstruction may be performed at the time of mastectomy or delayed until cancer treatment is complete. Immediate reconstruction avoids a flat chest after surgery, while delayed reconstruction allows time for healing and informed decision-making. Both approaches are safe when properly selected.
We treat patients from across Europe in a fully equipped hospital that meets European safety standards.
What is Breast Reconstruction?
Breast reconstruction recreates breast shape after mastectomy, lumpectomy, or breast injury. The goal is to restore a natural breast contour, projection, and symmetry with the opposite breast.
Reconstruction does not restore breast function or normal sensation. Reconstructed breasts do not produce milk, and sensation is usually reduced or absent. Despite this, reconstruction has well-documented benefits for body image, confidence, and overall quality of life after mastectomy.
Reconstruction can be performed using implants, the patient’s own tissue, or a combination of both. Implant-based reconstruction uses expanders and implants to form the breast mound. Autologous reconstruction uses tissue from areas such as the abdomen, back, or thighs to create a more natural breast. The appropriate approach depends on anatomy, cancer treatment, available tissue, and patient preference.
Most reconstructions are completed in stages. The initial surgery creates the breast mound, followed by procedures to refine shape, restore symmetry, and reconstruct the nipple-areola complex if desired. The full reconstruction process typically takes 6–12 months, depending on technique and the need for radiation therapy.


Candidates For Breast Reconstruction are patients with…

Types of Breast Reconstruction
Implant-Based Reconstruction
Implant-based reconstruction is usually performed in two stages. A tissue expander is placed beneath the chest muscle during or after mastectomy and gradually filled over several months to stretch the skin and muscle. The expander is then replaced with a permanent silicone or saline implant.
Autologous Tissue Flap Reconstruction
Flap reconstruction uses the patient’s own tissue—skin, fat, and sometimes muscle—from another body area to reconstruct the breast. Options include:
- DIEP flap: Lower abdominal tissue transferred while preserving muscle
- TRAM flap: Similar to DIEP but includes abdominal muscle
- Latissimus dorsi flap: Tissue from the upper back, often combined with an implant
- TUG flap: Inner thigh tissue for smaller reconstructions
- GAP flaps: Tissue from the buttocks when abdominal tissue is unavailable
Autologous reconstruction provides a natural look and feel, ages with the body, and avoids implant-related complications. It requires longer surgery (4–8 hours), donor-site scars, longer recovery (4–8 weeks), potential donor-site complications, and microsurgical expertise.
Hybrid Reconstruction
Hybrid reconstruction combines an implant with fat grafting. The implant provides volume, while fat grafting improves contour, softness, and overall shape.
Prepectoral vs. Submuscular Placement
Implants can be placed above the chest muscle (prepectoral) or beneath it (submuscular). Prepectoral placement avoids muscle disruption, while submuscular placement places the implant under the pectoralis major muscle. The choice depends on tissue quality and treatment history.
Breast reconstruction at Hygeia Plastic Surgery in Albania rebuilds breast shape and appearance following mastectomy for breast cancer treatment or prophylactic mastectomy for cancer prevention. This transformative surgery restores the breast mound, creating a natural-looking breast contour that helps women reclaim their sense of wholeness and confidence after the physical and emotional challenges of breast cancer and mastectomy.
Breast reconstruction can be performed immediately during mastectomy surgery or delayed until months or years after cancer treatment is complete. Multiple techniques are available including implant-based reconstruction using tissue expanders and permanent implants, or autologous tissue reconstruction using the patient’s own tissue from the abdomen, back, thighs, or buttocks to create a natural breast. The choice between immediate versus delayed reconstruction and implant versus autologous tissue depends on individual factors including cancer treatment plan, body type, tissue availability, radiation therapy requirements, and personal preferences regarding surgery complexity and recovery time.
At Hygeia Hospital in Tirana, our experienced plastic surgeons specialize in both implant-based and autologous tissue reconstruction, including advanced microsurgical flap procedures like DIEP flaps. We work closely with oncology teams to coordinate reconstruction timing with cancer treatment, ensuring optimal outcomes while prioritizing cancer care. Breast reconstruction is not just about physical restoration—it’s about helping women move forward after cancer with renewed confidence and the ability to feel whole again.
Key Information at a Glance
Surgery Time: 2-8 hours (varies by technique)
Anesthesia: General anesthesia
Hospital Stay: 2-7 days
Return to Work: 2-8 weeks
Full Recovery: 6-12 weeks
Cost in Albania: €4,500-14,000
Immediate vs. Delayed Reconstruction
One of the first decisions is whether to have reconstruction at the time of mastectomy (immediate) or wait until after cancer treatment is complete (delayed). Both approaches have advantages.
Immediate Reconstruction
Advantages:
Single anesthesia and recovery period, never experiencing life without a breast mound, potentially better aesthetic outcomes as skin envelope is preserved, fewer total surgeries, and psychological benefit of maintaining breast appearance continuity.
Considerations:
Longer initial surgery, need for reconstruction decision-making while processing cancer diagnosis, potential delays if complications occur before starting cancer treatment, and challenges if pathology reveals need for radiation.
Delayed Reconstruction
Advantages:
Time to focus on cancer treatment without reconstruction concerns, clearer understanding of whether radiation is needed (affecting reconstruction planning), time to research options and make informed reconstruction choices, and emotionally processing cancer before considering reconstruction.
Considerations:
Period of time living with mastectomy appearance, additional surgery with separate recovery period, potentially more challenging reconstruction due to scarring and tissue changes from cancer treatment.
Many women choose delayed reconstruction. There’s no time limit—reconstruction can be performed 5, 10, even 20+ years after mastectomy. What matters is when you feel ready.
Am I a Good Candidate?
Completed or planned mastectomy
You’ve undergone mastectomy or will undergo it as part of breast cancer treatment. Reconstruction is also performed for prophylactic mastectomy in high-risk women with BRCA mutations or strong family history.
Finished cancer treatment
For delayed reconstruction, cancer treatment should be complete with clearance from your oncologist. If planning immediate reconstruction, your cancer characteristics and treatment plan must be compatible with reconstruction.
Good general health
Reconstruction is major surgery requiring good overall health. Conditions like uncontrolled diabetes, significant cardiovascular disease, or immune disorders may preclude surgery or require careful management.
Realistic expectations
Understanding that reconstruction creates a breast mound but doesn’t restore original sensation, function, or exact appearance of your natural breast. Results are typically very good but imperfect.
Non-smoker
Smoking dramatically impairs healing, particularly problematic in flap reconstruction where tissue survival depends on blood supply. Must stop smoking at least 4-6 weeks before surgery.
Stable weight
Significant weight fluctuations affect reconstruction results, particularly autologous tissue reconstruction where breast size changes with body weight changes.
Personal motivation
You want reconstruction for yourself—to feel whole, restore confidence, eliminate need for external prosthesis. Pressure from others isn’t a good reason for elective surgery.
Adequate donor tissue
For autologous reconstruction, sufficient tissue at donor sites (abdomen, back, thighs, buttocks) is necessary. Very thin patients may not have adequate tissue for flap reconstruction.
Emotional readiness
You’ve processed the cancer diagnosis and treatment experience enough to engage with reconstruction decisions. Some women need time before feeling ready for more surgery.
Preparing for Reconstruction
Oncologic clearance
Your oncologist must clear you for surgery, confirming cancer treatment is complete and reconstruction won’t interfere with ongoing monitoring or treatment plans.
Smoking cessation
Stop all tobacco and nicotine products at least 4-6 weeks before surgery. This is absolutely critical for tissue survival in flap reconstruction and healing in all reconstruction types.
Medical optimization
Any chronic conditions (diabetes, hypertension) should be well-controlled. Complete any recommended cardiac or pulmonary testing.
Medication adjustments
Discontinue blood thinners, aspirin, NSAIDs, and supplements that affect clotting at least two weeks pre-surgery. Continue necessary medications unless specifically instructed otherwise.
Psychological preparation
Consider counseling or support groups for women undergoing reconstruction. Processing emotions before surgery helps with recovery and satisfaction.
Physical preparation
If planning flap reconstruction, core strengthening exercises (if cleared by your doctor) can aid recovery, particularly for abdominal flaps.
Arrange extensive support
Flap reconstruction requires significant assistance for 2-4 weeks. Arrange help with household tasks, childcare, transportation, and personal care.
Prepare recovery space
Set up comfortable resting area with pillows for positioning, entertainment, easy-access necessities. For flap reconstruction, prepare a recliner or adjustable bed for comfortable positioning.
Plan extended time off
Implant reconstruction typically requires 2-4 weeks off work; flap reconstruction 4-8 weeks depending on your job. Plan conservatively.
The Reconstruction Procedure
Reconstruction techniques vary significantly based on approach chosen.
Implant-Based Reconstruction
Tissue expander placement
Performed during mastectomy (immediate) or as separate surgery (delayed). After breast tissue removal, a tissue expander is placed either submuscularly or prepectorally. A small amount of saline is added initially. Incisions are closed and drains placed.
Expansion process
Beginning 2-4 weeks post-surgery, you return for expansion sessions every 1-2 weeks. Saline is injected through the expander’s port, gradually stretching skin and muscle. This continues until desired volume is achieved, typically slightly larger than final goal to allow for settling.
Expander-to-implant exchange
After expansion completion and a settling period (typically 2-3 months), exchange surgery replaces the expander with a permanent implant. This is a shorter surgery than initial placement. The implant pocket is refined, the expander removed, and permanent implant inserted.
Nipple reconstruction
Performed 3-6 months after implant exchange as a separate minor procedure, reconstructing nipple projection using local tissue flaps and tattooing areola color.
Autologous Tissue Flap Reconstruction (DIEP Flap Example)
Surgery takes 4-8 hours under general anesthesia. The breast surgeon performs mastectomy (if immediate reconstruction). The plastic surgeon harvests tissue from lower abdomen, identifying and carefully dissecting blood vessels (deep inferior epigastric perforators) that supply the tissue while preserving abdominal muscles.
The tissue flap—containing skin, fat, and blood vessels—is transferred to the chest. Using microsurgical techniques, the surgeon connects flap blood vessels to vessels in the chest (typically thoracodorsal or internal mammary vessels), re-establishing blood flow to the tissue. The flap is shaped into a breast mound and secured. The abdominal incision is closed, creating a tummy tuck result.
Drains are placed in both chest and abdomen. You’re monitored closely in recovery for 24-48 hours as blood flow to the flap is critical during early healing. Several months later (typically 3-6 months), refinement surgery addresses shape optimization, fat grafting, opposite breast symmetry, and nipple-areola reconstruction.
Recovery Timeline
Implant Reconstruction Recovery
Week 1: Moderate pain managed with medication. Drains remain in place (typically 7-14 days). Limited arm movement. Need significant assistance with daily activities.
Weeks 2-4: Pain decreasing. Drains removed. Gradual increase in arm movement and activities. Most patients return to desk work around week 3-4.
Weeks 4-8: Feeling much better. Restrictions on heavy lifting and strenuous activity gradually lift. Most activities resume by week 6-8.
Expansion visits: If tissue expander placed, expansion visits begin week 2-4 and continue every 1-2 weeks for 6-12 weeks.
Flap Reconstruction Recovery
Week 1: Significant pain and discomfort in both chest and donor site. Multiple drains in place. Strict bed rest with specific positioning to protect blood supply to flap. Unable to stand fully upright due to abdominal tightness (for abdominal flaps).
Weeks 2-3: Pain improving. Some drains removed. Beginning gentle walking, remaining hunched due to abdominal tightness. Still need considerable assistance.
Weeks 3-6: Progressing steadily. Able to stand more upright. Remaining drains removed. Activities gradually increasing.
Weeks 6-12: Significant improvement. Able to resume most normal activities. Returning to work for most jobs.
Months 3-6: Feeling much better. Breast mound settling into final shape. Swelling resolving.
Recovery from flap reconstruction is substantial—this is major surgery requiring significant commitment. However, most women feel the results are worth the recovery period.
Potential Risks and Complications
General surgical risks
Infection, bleeding/hematoma requiring drainage, poor wound healing, scarring, seroma (fluid collection), anesthesia risks, blood clots, and need for additional surgery.
Implant reconstruction specific risks
Capsular contracture (scar tissue tightening around implant), implant rupture or deflation, implant malposition, animation deformity with submuscular placement, rippling or visible implant edges, and loss of skin/tissue from expansion complications.
Flap reconstruction specific risks
Partial or complete flap loss due to blood supply compromise (rare but serious), fat necrosis (areas of flap tissue that don’t survive), abdominal weakness or hernia (with abdominal flaps), donor site complications (seroma, wound healing issues), and prolonged recovery period.
Radiation Impact
Prior or planned radiation significantly affects reconstruction outcomes. Radiation damages tissue, impairing healing and increasing complication rates. Implant reconstruction faces higher capsular contracture rates with radiation. Autologous tissue generally tolerates radiation better than implants.
If radiation is planned, many surgeons recommend delaying implant reconstruction until after radiation completion or choosing autologous tissue reconstruction.
Cost in Albania
Breast reconstruction at Hygeia Plastic Surgery in Albania varies significantly based on technique:
Implant-based reconstruction
€4,500-7,500 (including tissue expander placement, expansion process, and expander-to-implant exchange). Comparable procedures cost €12,000-20,000 in the UK, €13,000-22,000 in Germany, or €11,000-18,000 in Italy.
Autologous tissue flap reconstruction
€8,000-14,000 depending on flap complexity and whether microsurgical techniques are required. Comparable procedures cost €20,000-40,000+ in Western Europe.
Additional procedures
Nipple reconstruction and tattooing: €800-1,500 as a separate procedure.
Contralateral breast surgery: €2,500-4,500 depending on whether lift, reduction, or augmentation is needed for symmetry.
Pricing includes surgeon’s fee, anesthesia, hospital stay (typically 2-5 days for implant reconstruction, 5-7 days for flap reconstruction), all surgical supplies, post-operative garments, and initial follow-up appointments.
For International Patients
Factor in extended accommodation. Implant reconstruction requires 7-10 days in Albania initially, with return visits for expansion if placing expander. Flap reconstruction requires 10-14 days initially. The expander-to-implant exchange and subsequent procedures require additional trips or can be coordinated if you prefer to stay in Albania between stages.
Even with travel and extended accommodation, total costs remain 50-65% lower than having reconstruction at home.
Insurance & Payment Options
We provide transparent, itemized pricing during consultation. Insurance coverage varies—many European insurance policies cover reconstruction as part of breast cancer treatment. Check your specific policy and whether international treatment is covered.
Payment plans are available through medical finance providers. Contact our patient coordinators for specific financing options.
Combining with Other Procedures
Contralateral breast symmetry procedures
Often necessary to match the reconstructed breast. May include breast lift (mastopexy) if the opposite breast has sagged, breast reduction if the opposite breast is too large compared to reconstruction, or breast augmentation if the opposite breast is too small.
DIEP flap with tummy tuck
Abdominal flap reconstruction inherently includes a tummy tuck at the donor site—removing excess abdominal skin and fat while tightening abdominal wall.
Bilateral reconstruction
If mastectomy was performed on both breasts, bilateral reconstruction addresses both sides simultaneously or in staged procedures.
Prophylactic mastectomy
Women with BRCA mutations or strong family history may undergo prophylactic (preventive) mastectomy of unaffected breast(s) with immediate reconstruction to reduce cancer risk.
Fat grafting
Often used in subsequent procedures to refine reconstruction contour, improve upper pole fullness, soften edges, and optimize overall appearance.
Why Choose Hygeia Plastic Surgery?
Experienced reconstructive surgeons
Our board-certified plastic surgeons trained in both implant-based and autologous tissue reconstruction techniques. They understand the unique challenges and emotional aspects of post-mastectomy reconstruction.
Comprehensive approach
We perform the full spectrum of reconstruction options—tissue expanders, implants, flap reconstruction, fat grafting, nipple reconstruction—tailoring the approach to your individual circumstances.
Microsurgical expertise
Our surgeons trained in microsurgical techniques necessary for perforator flap procedures like DIEP flaps, offering the most advanced autologous reconstruction options.
Modern hospital facility
Hygeia operates as a fully equipped hospital with dedicated operating theatres, intensive care capabilities for monitoring flap reconstruction patients, and comprehensive support services.
European safety standards
Our facility meets European healthcare standards. We use CE-marked medical devices and follow international protocols for surgical safety.
Coordination with oncology teams
We work closely with your home-country oncologists and breast surgeons, ensuring seamless care continuity and communication throughout your reconstruction journey.
Compassionate care & medical tourism expertise
We understand that reconstruction is deeply personal and emotionally significant. Our team provides not just technical expertise but emotional support throughout your journey. We provide clear, detailed pricing with no hidden fees. Significant cost savings compared to Western Europe without compromising quality or safety. Our patient coordinators assist international patients with extended stays, accommodation recommendations, and all logistical aspects.
Breast reconstruction restores more than physical appearance—it restores confidence, wholeness, and the ability to move forward after cancer. At Hygeia, we’re committed to providing reconstruction that honors your journey and helps you reclaim your sense of self.
Meet the team



